Multimodality approach.
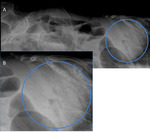
Since neither the symptoms of AMI nor the results of laboratory tests are specific enough for the accurate and early diagnosis, imaging plays an important role in the diagnosis and management of patients with AMI. Initial evaluation of less severely ill patients presenting to the ER with abdominal symptoms often starts with plain abdominal radiography (Fig. 15-18) and ultrasound (Fig 19-22).
The well-established first-line imaging modality for diagnosis of suspected AMI is multidetector CT. MDCT is the most sensitive (93.3%) and specific (95.9%) diagnostic tool for AMI [7]. Biphasic contrast-enhanced CT should include the whole abdomen, in both the arterial and the venous phases (Fig. 23).
Key imaging findings and diagnostic difficulties.
CT findings (Fig. 24-33) may correlate with type of AMI (Tab. 3.), provide information about the underlying pathophysiology (Tab. 5.) and are useful in excluding other causes of acute abdominal pain.
Combination of different CT findings allows the diagnosis of AMI with high sensitivity and specificity, however several other conditions, both benign and malignant, may produce similar findings (Tab. 6.).
Prognosis.
The prognosis for patients with AMI depends on prompt diagnosis (Tab. 5) and the underlying cause. Non-occlusive mesenteric ischemia (NOMI) accounting for approximately 20-30% of all the cases of AMI is associated with the highest rates of in-hospital mortality [9,10].
Early diagnosis and treatment have been reported to be the most important factors affecting mortality [3,15].
At one year after hospital admission due to AMI, only 26% of patients will remain alive. Most deaths occur during hospitalization and patients who are discharged have a good prognosis with 84 % alive at one year and 50–77 % at five years [7]. Higher in-hospital mortality is associated with older age, accompanying cardiac disease, acute renal failure, and simultaneous large bowel ischemia [15,17].
The most important prognostic factor in patients with AMI is intestinal viability (intraoperatively estimated from the colour of the intestinal segment, arterial pulsation, presence of bowel peristalsis and bleeding from the marginal arteries). Resection of all regions of non-viable intestine should be performed without delay [10]. If the physical exam demonstrates signs of peritonitis, there is likely irreversible intestinal ischemia with bowel necrosis [2]. CT features suggestive of intestinal necrosis should be always highlighted in the radiology report (Fig. 34.).




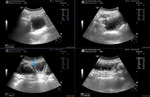

![Fig. 22: Color Doppler US shows significantly elevated peak systolic velocity (PSV) in celiac artery.
PSV >200 cm/s indicates a stenosis of greater than 70% with sensitivity, specificity, and positive predictive values of 75%, 89%, and 85% [18].](https://epos.myesr.org/posterimage/esr/ecr2020/156073/media/875054?maxheight=150&maxwidth=150)


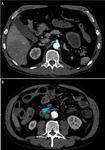
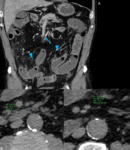

![Fig. 29: A 85-year-old female with atrial fibrillation presented to the emergency department with abdominal pain associated with nausea and vomiting.
Axial CT scans show intrahepatic portal gas (A) predominantly accumulating in the left lobe. Typically, hepatic portal vein gas is more peripherally located than gas due to pneumobilia and represents the propagation of intramural gas (B, arrowhead) through the mesenteric veins (B, arrows). This finding most often result from bowel wall necrosis and is associated with poor prognosis.
Patient underwent immediate surgery. Exploratory laparotomy revealed extensive small and large bowel necrosis. The benefits of extensive small bowel resection should be balanced against the resultant quality of life, morbidity, and mortality especially in elderly patients [7]. Surgeons decided to not perform bowel resection. Patient died one day after the onset of symptoms.](https://epos.myesr.org/posterimage/esr/ecr2020/156073/media/875648?maxheight=150&maxwidth=150)
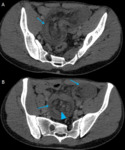

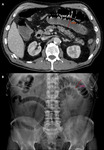
![Fig. 33: NOMI (secondary to hypotension) in a patient who suffered cardiac arrest during chemotherapy of diffuse non-Hodgkin lymphoma.
NOMI ischemia occurs due to severe vasoconstriction of mesenteric vessels supplying the intestine. Experimentally, it had been shown that bowel becomes ischemic when patient’s mean arterial pressure is <45 mmHg [2]. As a result of redistribution of blood flow to visceral organs findings of CT hypoperfusion complex include hyperenhancing bilateral adrenal glands (C) and kidneys (A). Interruption of the blood supply to the kidneys and liver causes infarction (A and B, blue arrows). Infarcts (ill-defined wedge-shaped areas of hypoattenuation which are mostly peripheral) are easily identified on post-contrast images. Hepatic infarction is an extremely rare situation and occurs when both hepatic arterial and portal vein flow are compromised.
The small bowel features are the most commonly observed findings in CT hypoperfusion complex. Pneumatosis intestinalis (D) is highly suggestive for bowel wall bowel necrosis and is associated with poor prognosis.](https://epos.myesr.org/posterimage/esr/ecr2020/156073/media/875760?maxheight=150&maxwidth=150)


![Table 7: Mortality of AMI based on Ernst Klar et al. [4].](https://epos.myesr.org/posterimage/esr/ecr2020/156073/media/875881?maxheight=150&maxwidth=150)


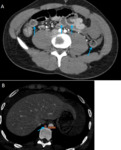
![Fig. 34: Imaging findings associated with high risk of bowel necrosis.
A: Axial CT scan (pulmonary window) showing the falciform ligament (arrow), outlined by intraperitoneal free gas (arrowhead). Irreversible ischemia leads to bowel wall necrosis and perforation. Pneumoperitoneum is the only pathognomonic finding of wall necrosis in patients with AMI [16].](https://epos.myesr.org/posterimage/esr/ecr2020/156073/media/888855?maxheight=150&maxwidth=150)
